Slipped Disc Treatment Without Surgery: Minimally Invasive Options Explained
April 20, 2026
CONTENTS
- Quick Answer
- Introduction
- Understanding the Spine and How a Disc “Slips”
- Why Surgery Is Rarely the First Option
- Conservative Slipped Disc Treatment in Singapore
- Minimally Invasive Options for Slipped Disc
- Where Does It Hurt? Interpreting Your Symptoms
- Red Flags That Need Urgent Assessment
- How Slipped Disc Is Diagnosed at Singapore Paincare
- A Pain Specialist’s Perspective
- Managing Slipped Disc Day-to-Day
- When Should You See a Slipped Disc Specialist in Singapore?
- Conclusion
- Frequently Asked Questions
- About Singapore Paincare
- Medical Disclaimer
Quick Answer
Most slipped discs in Singapore can be managed without open surgery. Non-surgical slipped disc treatment in Singapore typically starts with activity modification, physiotherapy, and targeted medication, then progresses to image-guided minimally invasive procedures such as epidural injections, nucleoplasty, or endoscopic laser decompression when conservative care is not enough. These options aim to decompress the nerve, calm inflammation, and restore function without the long recovery of traditional spinal surgery.
Introduction
Many Singaporeans first notice a slipped disc as a sharp, shooting pain down the leg after a long day at a desk, a heavy lift at the warehouse, or an awkward twist while carrying a child. The fear of “spinal surgery” can then loom larger than the pain itself. The good news is that open surgery is rarely the first answer. For most patients, slipped disc treatment in Singapore today revolves around non-surgical and minimally invasive options that aim to settle inflammation, decompress the pinched nerve, and restore movement without a large incision or long hospital stay.
This article walks you through what actually causes that disc-related pain, how doctors decide whether surgery is needed, and the full menu of minimally invasive treatments available in Singapore today. It is written to help you make a more informed decision when you sit down with a pain specialist.
Understanding the Spine and How a Disc “Slips”
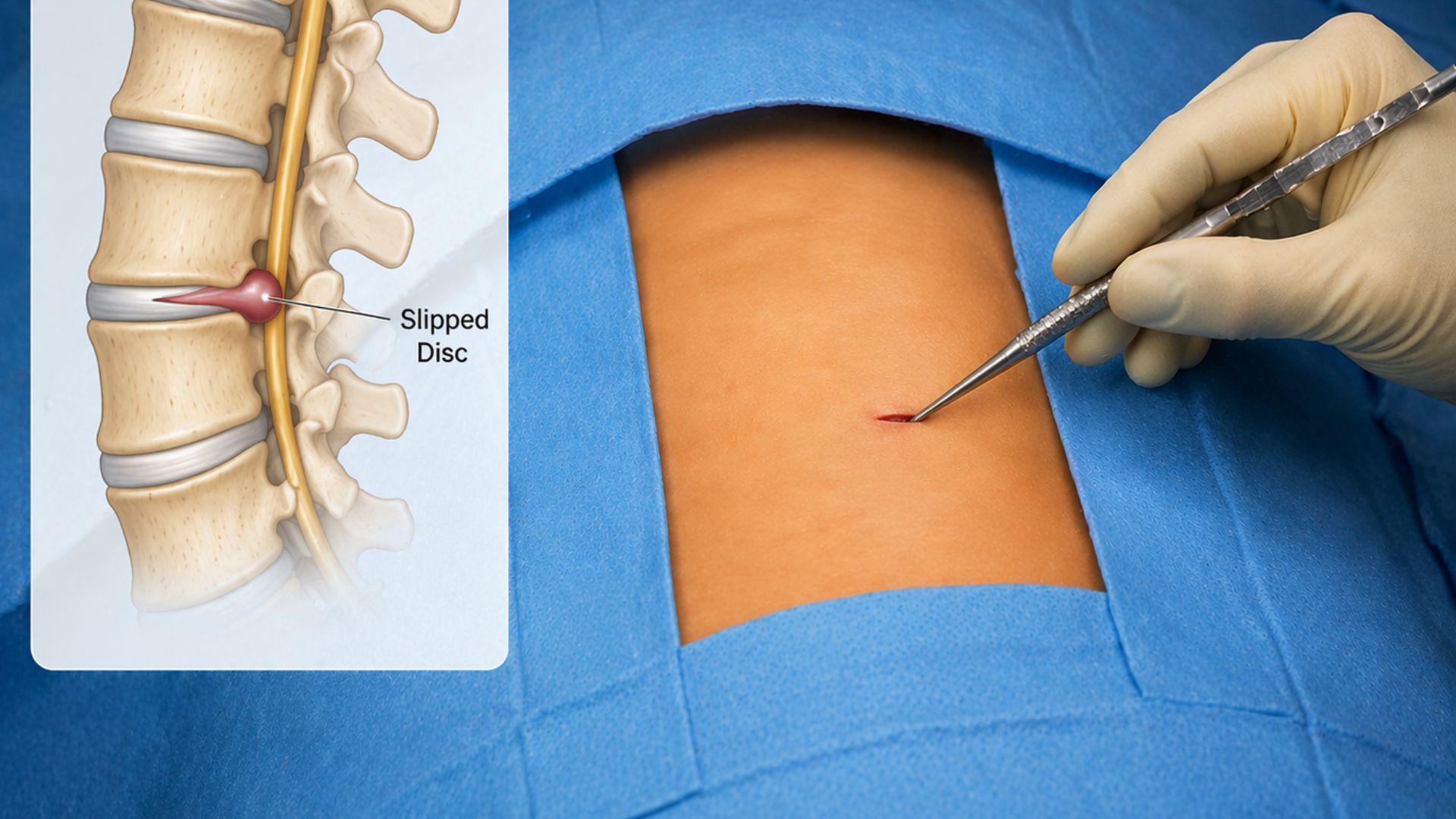
Your spine is a stack of bones called vertebrae, separated by soft, jelly-like cushions called intervertebral discs. Each disc has a tough outer ring (annulus fibrosus) and a softer inner core (nucleus pulposus). When the outer ring weakens, the inner core can bulge or leak out, pressing on the nerves nearby. That is what people call a “slipped disc”, though the disc does not literally slip out of place. Doctors more accurately call it a herniated, prolapsed, or protruding disc.
In Singapore, back pain is extremely common. The Ministry of Health lists low back pain among the leading reasons for outpatient primary care visits, and imaging studies show disc changes are especially frequent in adults aged 30 to 55. Long commuting hours on the MRT, desk-bound office work, and repetitive manual handling all contribute. The lumbar spine (lower back) bears most of the body’s weight during sitting and lifting, which is why it is the most common site for disc problems, followed by the neck.
Why Surgery Is Rarely the First Option
Open spine surgery, such as discectomy or spinal fusion, has a real role in clearly defined situations, particularly when there is severe nerve damage, progressive weakness, or loss of bladder and bowel control. However, published clinical guidance, including advice echoed by UpToDate and international spine societies, suggests that the majority of lumbar disc herniations improve with non-surgical care over weeks to months. Modern pain medicine adds a middle layer of treatment that sits between simple physiotherapy and full surgery, giving patients more options before committing to an operation.
This middle layer is where minimally invasive procedures (MIPs) come in. They are performed as outpatient or day procedures under local anaesthesia or light sedation, use small needles or 1 cm ports instead of open incisions, and allow most patients to return home the same day.
Conservative Slipped Disc Treatment in Singapore
Before any procedure is considered, most pain specialists begin with a conservative care pathway. This is not a delaying tactic. Many patients recover fully at this stage.
Activity Modification and Rest
Short periods of relative rest, avoiding aggravating postures, and modifying daily activities such as prolonged sitting or heavy lifting help calm the initial flare. Complete bed rest is not recommended. Gentle movement within pain limits actually speeds recovery.
Physiotherapy and Rehabilitation
A structured physiotherapy programme guides the spine through safe movement, strengthens the deep core and gluteal muscles that support the lumbar discs, and retrains posture. Manual therapy, traction, and progressive exercise are tailored to the specific level and direction of the disc bulge.
Anti-Inflammatory Medication
Short courses of NSAIDs such as diclofenac or celecoxib reduce inflammation around the irritated nerve root. For nerve-type pain with burning or electric-shock qualities, nerve stabilisers such as gabapentin or pregabalin, or low-dose antidepressants such as amitriptyline, may be used to quiet the overactive nerve signals. Opioids are reserved for short, carefully supervised use in severe pain.
Minimally Invasive Options for Slipped Disc
When pain persists despite conservative care, or when radiating leg or arm symptoms interfere with daily life, minimally invasive procedures offer targeted relief. At Singapore Paincare, these are selected through the Painostic® methodology, a three-protocol framework built on Diagnosis Formulation, Injection Roadmap, and Injection Technique. Diagnosis Formulation identifies the true pain generator, the Injection Roadmap sequences the most appropriate treatments, and the Injection Technique ensures precise, image-guided delivery to the affected structure.
Epidural Analgesia
An epidural steroid injection delivers a small, precise dose of steroid and local anaesthetic into the epidural space around the inflamed nerve root. It reduces swelling, calms nerve irritation, and can give days to weeks of relief, often creating the window needed for physiotherapy to take hold. It is one of the most commonly used and well-studied non-surgical slipped disc treatments.
Peripheral Nerve Block
A diagnostic and therapeutic nerve block uses local anaesthetic and an anti-inflammatory agent placed near a specific nerve or nerve bundle. Apart from giving relief, it helps confirm which nerve is driving the pain, which is especially useful when scans show changes at more than one spinal level.
Nucleoplasty
Nucleoplasty uses controlled plasma energy to gently remove a small amount of the disc’s inner core through a fine needle. This decompresses the herniated disc from the inside, taking pressure off the nerve root. It is particularly suitable for contained disc herniations with predominant radicular (leg or arm) pain and is performed under local anaesthesia as a day procedure.
Neuroplasty
Neuroplasty involves passing a small catheter into the narrowed section of the spine to mechanically break down scar tissue and adhesions around the trapped nerve, then delivering anti-swelling medication directly to the site. It is helpful where chronic inflammation and adhesions are contributing to ongoing nerve pain, including after previous spine interventions.
Endoscopic Laser Decompression
In endoscopic laser decompression, a rigid 1 cm port with a camera is inserted into the spine. Under direct vision, laser or radiofrequency energy is used to precisely remove bone spurs and portions of the herniated disc tissue that are compressing the nerve. It bridges the gap between injection-based decompression and open surgery, offering a true decompressive procedure through a small skin puncture.
Radiofrequency Ablation and Pulsed Radiofrequency
When the main pain generator is the facet joint irritated by the disc change, rather than the nerve root itself, radiofrequency ablation (RFA) uses heat to disrupt the small pain-carrying nerves to the facet joint. Pulsed radiofrequency (PRF) is a lower-temperature variant used around nerve roots to desensitise them without ablation. Both can give several months of relief and are suitable for patients with confirmed facet-mediated pain.
For a more detailed explanation of how these treatments are combined for disc-related pain, see Singapore Paincare’s slipped disc treatment in Singapore page, and the related sciatica resource for patients with leg-dominant symptoms.
Where Does It Hurt? Interpreting Your Symptoms
The location of the pain often tells a doctor a lot about which disc is involved. A lumbar disc at the L4/L5 level commonly radiates pain down the outer thigh and calf into the top of the foot and big toe, sometimes with weakness in lifting the foot. An L5/S1 disc tends to send pain down the back of the thigh and calf into the outer foot and little toe. Cervical disc problems can send pain from the neck into the shoulder blade, down the arm, and into specific fingers, often with pins-and-needles sensations.
Pain that is worse on sitting, bending forward, coughing, or sneezing, and that eases with walking or lying down, is classically disc-related. Pain that is sharper on standing and walking, and relieved by sitting, often points more toward spinal stenosis or facet-related problems. These patterns are a guide only, and a proper clinical assessment is needed to confirm the source.
Red Flags That Need Urgent Assessment
Most slipped discs are not emergencies. However, the following symptoms should prompt urgent medical attention rather than waiting:
- New or worsening weakness in a leg or arm, especially foot drop or difficulty gripping
- Numbness in the inner thighs, buttocks, or groin (saddle anaesthesia)
- Loss of bladder or bowel control, or difficulty passing urine
- Severe pain that does not settle at all with rest or medication
- Fever, unexplained weight loss, or a history of cancer alongside new back pain
These red flags may signal cauda equina syndrome, spinal infection, or tumour, and need prompt evaluation at an emergency department.
How Slipped Disc Is Diagnosed at Singapore Paincare
Diagnosis begins with a detailed pain history and physical examination. The specialist asks about the nature, location, triggers, and radiation of pain, as well as how it affects work, sleep, and mood. A neurological examination tests strength, sensation, reflexes, and nerve-tension signs.
Imaging, most commonly MRI, helps confirm the level and size of the disc herniation and rule out other causes such as tumours or infection. However, MRI findings on their own are not enough. Many people without pain also show disc bulges on imaging. This is where the Painostic® methodology adds depth through its three protocols. Diagnosis Formulation combines the history, examination, and imaging into a clear pain picture. The Injection Roadmap then sequences the most appropriate interventions. Injection Technique ensures precise delivery to the affected anatomy. Diagnostic nerve blocks may be used to confirm which structure is responsible before a definitive treatment is chosen.
A Pain Specialist’s Perspective
In clinic, one of the most common patterns seen in Singapore patients is the “MRI-pain mismatch”. A working professional in their 40s comes in with a six-month history of leg pain. The MRI shows a small L4/L5 disc bulge, and they are told surgery is not clearly indicated, but also that “nothing else can be done”. They arrive exhausted, on escalating painkillers, and convinced the only remaining option is fusion surgery.
The more useful question is not “how big is the bulge” but “which structure, at which level, is actually generating this pain right now”. A careful history often reveals that the pain worsens specifically with sitting and forward bending, that it follows a clear L5 dermatomal pattern, and that there is a subtle positive straight-leg raise on one side. A targeted transforaminal epidural injection, combined with a structured rehabilitation plan, can settle the flare and allow recovery without any need for surgery. In a smaller subset, nucleoplasty or endoscopic decompression is added when pain remains mechanical and nerve-dominant.
The clinical takeaway is that waiting for a disc problem to “declare itself” rarely helps. Pain lasting more than four to six weeks, especially with leg or arm symptoms, deserves a dedicated pain-specialist assessment rather than another repeat MRI.
Managing Slipped Disc Day-to-Day
While treatment is ongoing, small daily habits make a real difference. Keeping moving within comfortable limits, rather than long periods of complete rest, tends to help discs recover. Short walking breaks every 30 to 45 minutes during desk work reduce sustained loading on the lumbar spine. Lifting with the knees bent and the object close to the body, sleeping with a pillow between or under the knees, and maintaining a healthy body weight all reduce mechanical strain.
Gentle core and gluteal strengthening, once approved by a physiotherapist, support the spine from the inside. Smoking is associated with faster disc degeneration and should ideally be reduced or stopped. These are supportive measures, not substitutes for a proper diagnosis.
When Should You See a Slipped Disc Specialist in Singapore?
You should consider seeing a slipped disc specialist in Singapore when back or neck pain has not settled after two to four weeks of conservative care, when pain is radiating into a leg or arm, when there is any new numbness or weakness, or when the pain is significantly affecting sleep, work, or mood. No referral is needed to see a pain specialist in Singapore. An earlier assessment means an earlier, more targeted plan, and often a faster return to normal activity.
To understand which treatment might be most appropriate for your situation, visit the Singapore Paincare slipped disc treatment in Singapore page for an overview, or speak to a pain specialist to find out if a minimally invasive option is right for you.
Conclusion
A slipped disc does not automatically mean surgery. With accurate diagnosis and a graduated treatment pathway, most patients in Singapore improve with a combination of conservative care and minimally invasive procedures. The key is not how the scan looks, but how carefully the pain is matched to the right treatment. If back or nerve pain is affecting your daily life, speak to a pain management team to explore your options and build a plan that avoids unnecessary surgery while still addressing the root cause.
Frequently Asked Questions
Can a slipped disc heal without surgery?
Yes, the majority of slipped discs improve without surgery. With a combination of activity modification, physiotherapy, medication, and where needed, minimally invasive procedures such as epidural injections or nucleoplasty, most patients regain function over weeks to months. Surgery is usually reserved for cases with severe or progressive nerve damage, loss of bladder or bowel control, or pain that fails all other treatments.
How long does slipped disc pain last?
Acute slipped disc pain typically settles within four to six weeks for many patients, although residual symptoms can linger for several months. Recovery depends on the size and location of the herniation, overall fitness, occupation, and how quickly appropriate treatment is started. Pain lasting longer than six weeks, or with any leg or arm weakness, warrants assessment by a pain specialist.
What are the red flags for a slipped disc?
Red flags include new or worsening weakness in a limb, numbness around the groin or inner thighs, loss of bladder or bowel control, severe pain that does not respond to rest or medication, and systemic symptoms such as fever or unexplained weight loss. These may signal serious conditions like cauda equina syndrome or infection, and require urgent medical evaluation at an emergency department.
What non-surgical slipped disc treatments are available in Singapore?
Non-surgical slipped disc treatment in Singapore typically includes physiotherapy, anti-inflammatory and nerve-pain medication, epidural steroid injections, peripheral nerve blocks, nucleoplasty, neuroplasty, endoscopic laser decompression, and radiofrequency ablation for facet-related pain. The right combination depends on the level of the disc, symptom pattern, and the individual’s response to earlier treatment.
How is a slipped disc diagnosed at Singapore Paincare?
At Singapore Paincare, diagnosis combines a detailed pain history, physical and neurological examination, MRI where indicated, and diagnostic injections. The Painostic® methodology is built on three protocols: Diagnosis Formulation, which identifies the true pain generator; the Injection Roadmap, which sequences the most appropriate treatments; and Injection Technique, which ensures precise delivery of medication to the affected structure.
About Singapore Paincare
Singapore Paincare Medical Group is an SGX-listed pain management group offering specialist-led diagnosis and minimally invasive treatment for acute and chronic pain. Through the proprietary Painostic® methodology, the group provides integrated care across pain medicine, physiotherapy, rehabilitation, and allied services from clinics at Paragon and Novena.
Medical Disclaimer
This article is intended for general informational purposes only and does not constitute medical advice. Please consult a qualified healthcare professional for diagnosis and treatment tailored to your individual condition.