What Is Backbone Disc Displacement and How Does It Affect Your Daily Life?
April 21, 2026
CONTENTS
- Introduction
- What Backbone Disc Displacement Really Means
- Why Discs Displace: Common Causes in Singapore
- Where Does It Hurt? Interpreting Your Symptoms by Location
- Symptoms That Often Accompany Disc Displacement
- How Disc Displacement Affects Your Daily Life
- How Disc Displacement Is Diagnosed
- Slipped Disc Treatment in Singapore: Your Options for Disc Displacement
- A Pain Specialist’s Perspective
- Managing Backbone Disc Displacement Day-to-Day
- When Should You See a Pain Specialist in Singapore?
- Conclusion
- Frequently Asked Questions
Quick Answer: Backbone disc displacement, more commonly called a slipped or herniated disc, is when the soft inner core of a spinal disc pushes against or through its outer ring and irritates nearby nerves. It often causes back or neck pain, leg or arm numbness, and reduced mobility. In Singapore, it commonly affects office workers, manual workers, and older adults, and can disrupt sitting, sleep, driving, exercise, and daily activities. Effective non-surgical slipped disc treatment in Singapore is available through pain specialists.
Introduction
When a specialist first mentions “disc displacement”, many patients are surprised. They have lived with dull low back aches for years, with the occasional sharp twinge, and assumed it was just age or a bad posture habit. The idea that something in the spine has actually shifted can sound frightening. The truth is more reassuring. Disc displacement is usually a manageable structural issue, and modern slipped disc treatment in Singapore covers a wide range of non-surgical options, especially when caught early.
This article explains what backbone disc displacement actually is, how it affects daily life in ways most patients do not realise, how it is diagnosed, and what options exist in Singapore to treat it without jumping straight to surgery.
What Backbone Disc Displacement Really Means
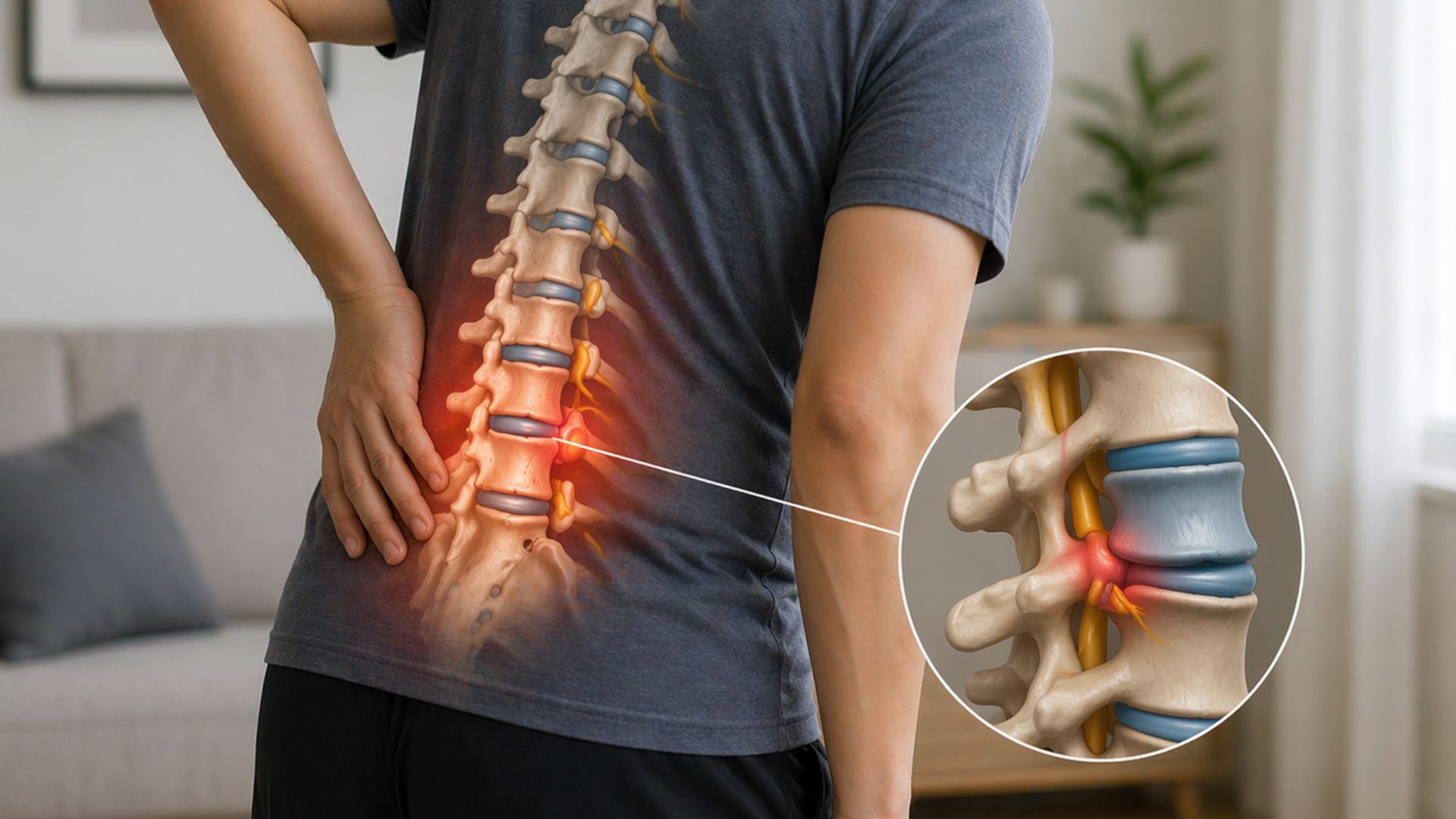
Your backbone, or spine, is made up of 33 bones called vertebrae, separated by cushioning discs. Each disc has a tough outer ring, called the annulus fibrosus, and a soft gel-like centre, called the nucleus pulposus. These discs act as shock absorbers during movement, allow the spine to bend and twist, and keep the vertebrae from grinding against each other.
“Backbone disc displacement” is a general term that covers several related problems. Bulging discs occur when the outer ring weakens and the disc pushes outward slightly. Herniated or prolapsed discs occur when the inner core pushes through a tear in the outer ring. Extruded or sequestered discs occur when part of the inner core breaks away from the disc entirely. Any of these can irritate nearby nerves. Depending on which nerve is affected, you may feel pain, tingling, numbness, or weakness in different parts of the body.
In Singapore, low back pain and neck pain are among the leading causes of years lived with disability, according to Ministry of Health data. Imaging studies show that disc-related changes are particularly common in adults between 30 and 55, though they can occur at any age.
Why Discs Displace: Common Causes in Singapore
Discs do not usually displace from a single dramatic event. More often, they fail gradually over years of repetitive loading, then tip into symptoms during one particular movement.
Age-Related Disc Wear
From our mid-20s, discs begin to lose water content, which makes them less elastic and more prone to tearing. This is a normal ageing process, though its rate varies widely between individuals.
Prolonged Sitting and Desk Work
Extended sitting, especially slouched over a laptop or phone, loads the lumbar and cervical discs in a flexed position. Many office workers in Singapore sit for over eight hours a day, and the cumulative load contributes to disc stress over years.
Heavy Lifting and Awkward Postures
Lifting heavy items with a bent spine or twisted torso, common in warehousing, construction, nursing, and caregiving, places high shear stress on discs. Even single incidents of improper lifting can cause a disc to herniate if the outer ring is already weakened.
Sudden Trauma
Falls, road traffic accidents, and sports injuries can cause acute disc herniation. In Singapore, this is often seen after cycling, badminton, or weekend football injuries, as well as workplace accidents.
Genetic and Lifestyle Factors
Family history plays a role in disc structure and strength. Smoking, obesity, and low physical conditioning all increase the risk of symptomatic disc displacement, as do pregnancy and postpartum recovery in women.
Repetitive Movements
Long-haul drivers, hairdressers, chefs, dentists, and others who repeat specific postures or movements through the day often develop disc wear at predictable levels of the spine.
Where Does It Hurt? Interpreting Your Symptoms by Location
The location of pain often tells a pain specialist a lot about which disc is affected. Cervical (neck) disc problems commonly send pain from the neck into the shoulder blade, down the outer arm, and into the fingers. Pins-and-needles sensations are common. Patients may struggle to turn the head fully to one side, or notice weakness when gripping a cup.
Thoracic (mid-back) disc problems are less common. They can cause band-like pain around the chest or ribs, sometimes mistaken for heart or lung issues. Lumbar (lower back) disc problems are the most frequent. An L4/L5 disc may radiate pain along the outer thigh and calf into the top of the foot. An L5/S1 disc tends to send pain down the back of the leg into the outer foot.
Pain that worsens on sitting, bending forward, coughing, or sneezing is classic for disc involvement. Pain that eases on lying down and worsens with long standing may still be disc-related, though other causes must be considered. These patterns are a guide only and do not replace a clinical assessment.
Symptoms That Often Accompany Disc Displacement
Beyond the pain itself, displaced discs often produce a cluster of symptoms that quietly reshape how you live. Patients frequently describe morning stiffness that eases with light movement. They also describe difficulty standing up straight after prolonged sitting. An awkward shifted posture (sometimes called a sciatic list) can develop to protect the irritated nerve.
Numbness, tingling, or a “pins and needles” sensation in a specific area of the leg, foot, arm, or hand points toward nerve root involvement. Muscle weakness indicates a more significant nerve compression. Signs include difficulty lifting the front of the foot (foot drop), weak grip, or trouble rising from a squat. Some patients also notice that their leg or arm feels “heavy” or “dead” during certain activities.
Red Flags That Need Urgent Medical Attention
Most disc problems are not emergencies. However, the following symptoms need urgent evaluation, ideally at an emergency department:
- New or rapidly worsening weakness in a leg or arm
- Numbness around the groin, buttocks, or inner thighs (saddle anaesthesia)
- Loss of bladder or bowel control, or difficulty passing urine
- Severe, unrelenting pain that does not respond to rest or medication
- Back pain after significant trauma such as a fall or motor-vehicle accident
- Back pain with fever, chills, or unexplained weight loss
These may signal cauda equina syndrome, infection, fracture, or tumour, and require prompt assessment.
How Disc Displacement Affects Your Daily Life
The pain itself is often only part of the story. Over weeks and months, disc displacement reshapes small daily decisions in ways many patients do not consciously notice until they look back.
Work and Productivity
Sitting through long meetings becomes uncomfortable. Typing at a desk triggers shoulder and arm pain. Concentration drops as background pain competes for attention. Patients with manual jobs may avoid lifting or bending, or push through with workarounds that strain other joints. Absenteeism and reduced productivity are well-documented in the Singapore workforce in relation to chronic back and neck pain.
Sleep and Energy
Disc-related pain often worsens at night, particularly when lying in certain positions or turning in bed. Poor sleep then feeds into fatigue, irritability, and lowered pain tolerance the next day, creating a cycle that is difficult to break without targeted treatment.
Exercise and Hobbies
Activities like running, golf, badminton, yoga, and gym training are often scaled back or abandoned. This loss of fitness further weakens the core and postural muscles that normally support the spine, which can worsen the disc problem over time.
Driving, Travel, and Commuting
Long commutes on the MRT or long drives become an ordeal. Some patients avoid long-haul flights or family trips because of the pain associated with prolonged sitting.
Mood, Relationships, and Mental Health
Chronic pain is closely linked to anxiety, low mood, and social withdrawal. Patients may become irritable at home, reluctant to join family outings, or anxious about whether they will “damage” their spine with certain movements. This is why the Painostic® methodology used at Singapore Paincare starts by understanding how pain is actually affecting the patient’s daily life. It uses three protocols: Diagnosis Formulation, Injection Roadmap, and Injection Technique. Each protocol looks beyond the scan to the real-world impact on work, sleep, and movement.
How Disc Displacement Is Diagnosed
Diagnosis starts with a careful history and physical examination, not an immediate rush to MRI. The specialist asks about the timing and character of pain, what triggers and eases it, and how it radiates. Physical examination tests strength, sensation, reflexes, and nerve-tension signs such as the straight-leg raise.
Imaging, most commonly MRI, helps confirm the level and size of any disc displacement. It also rules out other causes such as tumours, fractures, or infection. However, MRI findings alone are not always conclusive. Many adults without pain show disc changes on imaging.
At Singapore Paincare, the Painostic® methodology is built on three protocols. Diagnosis Formulation integrates history, examination, and imaging to identify the true pain generator. The Injection Roadmap sequences treatments from the least to the most invasive. Injection Technique ensures precise delivery of medication to the target structure. Diagnostic nerve blocks may be used to confirm which nerve or joint is driving the pain before a definitive plan is set.
Slipped Disc Treatment in Singapore: Your Options for Disc Displacement
Most patients with backbone disc displacement improve without surgery. The treatment pathway is typically graduated, starting with the least invasive effective option.
Activity Modification and Rest
Short periods of relative rest and avoidance of aggravating postures settle the initial flare. Complete bed rest is not recommended. Gentle movement within comfortable limits tends to speed recovery.
Physiotherapy and Rehabilitation
Structured physiotherapy retrains posture and movement, strengthens deep core and gluteal muscles, and progressively restores safe loading of the spine.
Anti-Inflammatory Medication
Short courses of NSAIDs calm inflammation around the irritated nerve. For nerve-type pain, stabilisers such as gabapentin or pregabalin, or low-dose antidepressants such as amitriptyline, may be used. Opioids are used sparingly and only for severe short-term pain under supervision.
Epidural Analgesia
An image-guided epidural steroid injection delivers a targeted dose of steroid and local anaesthetic around the inflamed nerve root, reducing swelling and creating a window for rehabilitation to progress.
Peripheral Nerve Block
A nerve block uses local anaesthetic and anti-inflammatory medication placed near a specific nerve or bundle, both confirming the pain source and providing relief.
Nucleoplasty
Nucleoplasty decompresses a contained herniated disc from the inside, using controlled plasma energy delivered through a fine needle under local anaesthesia. It is particularly suitable for patients with persistent radicular pain despite conservative care.
Neuroplasty
Neuroplasty uses a small catheter to break down scar tissue and adhesions around an impinged nerve, then delivers anti-swelling medication directly to the site.
Endoscopic Laser Decompression
For more substantial decompression without open surgery, endoscopic laser decompression uses a 1 cm port with a camera to allow direct-vision laser removal of bone spurs and displaced disc tissue.
Radiofrequency Ablation
When facet joint irritation is the dominant pain source alongside a disc change, radiofrequency ablation disrupts the small pain-carrying nerves supplying the facet joint, giving months of relief.
You can read more about these options on Singapore Paincare’s slipped disc treatment in Singapore page, and on the dedicated lower back pain resource for patients whose symptoms sit mostly in the lumbar region.
A Pain Specialist’s Perspective
A common pattern we see in Singapore clinic involves two very different patient profiles presenting with the same diagnosis. The first is a 35-year-old tech professional who develops sudden lumbar pain after lifting gym equipment, with a sharp L5 dermatomal pain radiating down the leg. The MRI shows a clear extruded disc. The second is a 58-year-old business owner with years of dull lower back stiffness, who now notices aching calves on long walks and needs to pause on the way to the MRT. Imaging shows multi-level disc bulges, mild spinal stenosis, and facet changes.
Both are, technically, “disc displacement” patients. But their clinical picture, pain generator, and best treatment pathway are quite different. The younger patient often responds well to a transforaminal epidural injection, rehabilitation, and occasionally nucleoplasty. The older patient may benefit more from a combination approach, including facet-joint RFA, Pulsed Radiofrequency, and targeted rehabilitation to address deconditioning.
The takeaway is that treating “a slipped disc” based on the scan alone rarely works. Outcomes improve when treatment is matched to the pain pattern, patient goals, and functional limitations, not to the label on the imaging report. Early, accurate assessment matters because waiting rarely clarifies the picture. It more often allows deconditioning and nerve sensitisation to set in.
Managing Backbone Disc Displacement Day-to-Day
Small habits can meaningfully support recovery. Keeping moving within comfortable limits, rather than long stretches of complete rest, tends to help discs recover. Standing up and walking briefly every 30 to 45 minutes during desk work reduces sustained loading on the lumbar spine. Lifting with bent knees and keeping the object close to the body, sleeping with a pillow between or under the knees, and maintaining a healthy body weight all reduce mechanical strain on the discs.
Gentle core and gluteal strengthening, once cleared by a physiotherapist, supports the spine from the inside. Stopping smoking is associated with slower disc degeneration. Managing stress and sleep quality also improves pain tolerance. These are supportive measures, not substitutes for a proper diagnosis.
When Should You See a Pain Specialist in Singapore?
Consider seeing a pain specialist if back or neck pain has not settled after two to four weeks of self-care, if pain is radiating into a leg or arm, if there is new numbness or weakness, or if the pain is affecting your sleep, work, or mood. No referral is needed in Singapore, and earlier assessment typically leads to a more targeted plan and a faster return to normal activity.
Find out more about your options. Consult a back pain specialist in Singapore today via the Singapore Paincare slipped disc treatment page.
Conclusion
Backbone disc displacement sounds alarming, but for most patients it is a treatable structural issue rather than a life sentence of pain. What matters is recognising how it is affecting your daily life, from work and sleep to exercise and mood, and getting a careful diagnosis before the pain rewires your routine. With the right combination of conservative care and minimally invasive treatment, many patients in Singapore regain the activities they had quietly given up. Speak to a pain management specialist to find out which path is most appropriate for your situation.
Frequently Asked Questions
Is disc displacement the same as a slipped disc?
Yes, in general usage. “Backbone disc displacement”, “slipped disc”, “herniated disc“, and “prolapsed disc” are often used interchangeably to describe a disc whose inner core has pushed against or through its outer ring. Doctors may use more specific terms such as bulging, protrusion, extrusion, or sequestration to describe the degree of displacement on imaging. The treatment principles are similar, though the details depend on the level, severity, and symptoms.
Can disc displacement heal on its own?
Many mild to moderate disc displacements do settle over weeks to months, especially with appropriate rest, activity modification, and physiotherapy. The body can reabsorb small disc herniations over time and the inflammation around the nerve can subside. However, larger herniations, persistent nerve compression, or recurring episodes often benefit from specialist input and targeted minimally invasive treatment to avoid chronic pain and nerve sensitisation.
What daily activities should I avoid with a slipped disc?
During an acute flare, avoid heavy lifting, twisting while lifting, prolonged sitting or driving without breaks, and high-impact activities such as running or contact sports. Gentle walking, light stretching, and movement within comfortable limits are usually encouraged. As pain settles, most activities can be reintroduced progressively under the guidance of a physiotherapist. Individual advice should be based on your specific diagnosis.
How long does it take to recover from backbone disc displacement?
Many acute flares settle within four to six weeks, although residual symptoms can linger for several months. Recovery depends on the size and level of the herniation, overall fitness, occupation, and how quickly appropriate treatment is started. Patients with leg or arm symptoms, or with pain persisting beyond six weeks, should be assessed by a back pain specialist to avoid prolonged nerve irritation and chronic pain.
What is the best treatment for a slipped disc in Singapore?
There is no single best treatment. The most effective approach depends on the level of the disc, the specific nerve involved, symptom pattern, and the patient’s goals. In Singapore, back pain treatment typically starts with conservative care and graduates to minimally invasive procedures such as epidural injections, peripheral nerve blocks, nucleoplasty, neuroplasty, or endoscopic laser decompression if needed. Pain specialists use the Painostic methodology to match the treatment to the actual pain generator rather than treating the scan alone.