What Are the Symptoms of Fibromyalgia?
Fibromyalgia symptoms can vary widely between individuals and fluctuate over time depending on activity, stress, and sleep quality. The two defining features are widespread pain and persistent fatigue, but most patients experience a broader constellation of symptoms.
Important: Pain intensity in fibromyalgia typically worsens after disrupted sleep, during high-stress periods, or following physical overexertion. If these patterns are familiar, a pain specialist assessment is warranted.
What Causes Fibromyalgia?
The precise cause of fibromyalgia remains under investigation, but the current scientific consensus points to central sensitisation — a state in which the central nervous system becomes hypersensitive to pain signals, amplifying normal sensations into severe pain experiences. Fibromyalgia is broadly classified into two forms — primary and secondary — each with distinct underlying drivers.
Primary Fibromyalgia
Primary fibromyalgia is the more common form. It is considered a dysfunctional disorder — arising from a constellation of biological responses to stress in individuals who are genetically or psychologically more susceptible. No single external cause can be identified, which is why this form is sometimes referred to as idiopathic fibromyalgia.
Contributing factors in primary fibromyalgia include:
| Contributing Factor | How It Plays a Role |
|---|---|
| Genetics & Family History | Studies show that 28% of children whose mothers have fibromyalgia also develop the condition. Among children with fibromyalgia, 66% of their parents reported some form of chronic pain. Both genetic predisposition and shared family coping patterns appear to contribute. |
| Chronic Sleep Disruption | Disrupted deep sleep triggers immune system factors associated with inflammation and heightened pain sensitivity. In one study, volunteers without fibromyalgia reported fibromyalgia-like pain after sustained sleep disruption, suggesting disordered sleep may be an original precipitating factor in many cases. |
| Neurochemical Abnormalities | Reduced serotonin and tryptophan levels, elevated substance P in cerebrospinal fluid, and abnormalities in the hypothalamus-pituitary-adrenal (HPA) axis all alter pain modulation and contribute to central sensitisation. People with fibromyalgia also tend to have lower magnesium levels. |
| Psychosocial Stress & Trauma | Prolonged psychosocial stress, emotional or physical abuse, and PTSD are recognised triggers, particularly relevant in patients presenting after severe accidents or ongoing emotional distress. Hypervigilance, a generalised amplification of sensation caused by trauma, can lower the pain threshold significantly. |
| Gender | Fibromyalgia is two to six times more common in women than men, with most cases presenting between ages 35 and 55. Symptoms are typically more severe in women. |
| Muscle Cell Abnormalities | Some research has identified lower levels of muscle-cell enzymes (phosphocreatine and ATP) in fibromyalgia patients, impairing the muscle’s ability to relax after contraction. This can create a self-reinforcing loop of muscle atrophy, pain, and reduced physical activity. |
Secondary Fibromyalgia
Secondary fibromyalgia develops as a consequence of a specific, identifiable underlying condition — such as a physical injury, autoimmune disorder (e.g. rheumatoid arthritis, lupus), or surgical event. The symptoms are clinically identical to primary fibromyalgia but are often more difficult to treat because the underlying condition continues to act as a driver.
Clinical note: In one study, secondary fibromyalgia developed in over 20% of patients who had sustained neck injuries. If you have a pre-existing rheumatic or autoimmune condition and are now experiencing widespread pain, a pain specialist evaluation is important — fibromyalgia can co-exist with and complicate these conditions.
How Is Fibromyalgia Diagnosed in Singapore?
There is no single blood test or imaging scan that confirms fibromyalgia. Diagnosis is clinical — based on the American College of Rheumatology (ACR) criteria — and requires a comprehensive evaluation by a pain specialist. Standard laboratory tests in fibromyalgia are typically normal; abnormal results usually indicate that another condition should be investigated instead.
The ACR Diagnostic Criteria
According to the American College of Rheumatology’s criteria for diagnosing fibromyalgia, a clinical diagnosis of fibromyalgia, the following must be present:
- Widespread pain lasting at least 3 months, occurring in upper and lower body, on both left and right sides, and in the spine
- Intense pain (not just tenderness) when firm pressure is applied to at least 11 of 18 defined tender point sites
- Associated symptoms including fatigue, non-restorative sleep, and cognitive difficulties
- Exclusion of other conditions that can produce similar symptoms
Some specialists apply a modified threshold — diagnosing fibromyalgia with only 8 to 10 tender points when the patient also presents with at least three of the following: morning stiffness, fatigue, sleep disturbance, numbness or tingling in the hands and feet, or recurrent headaches.
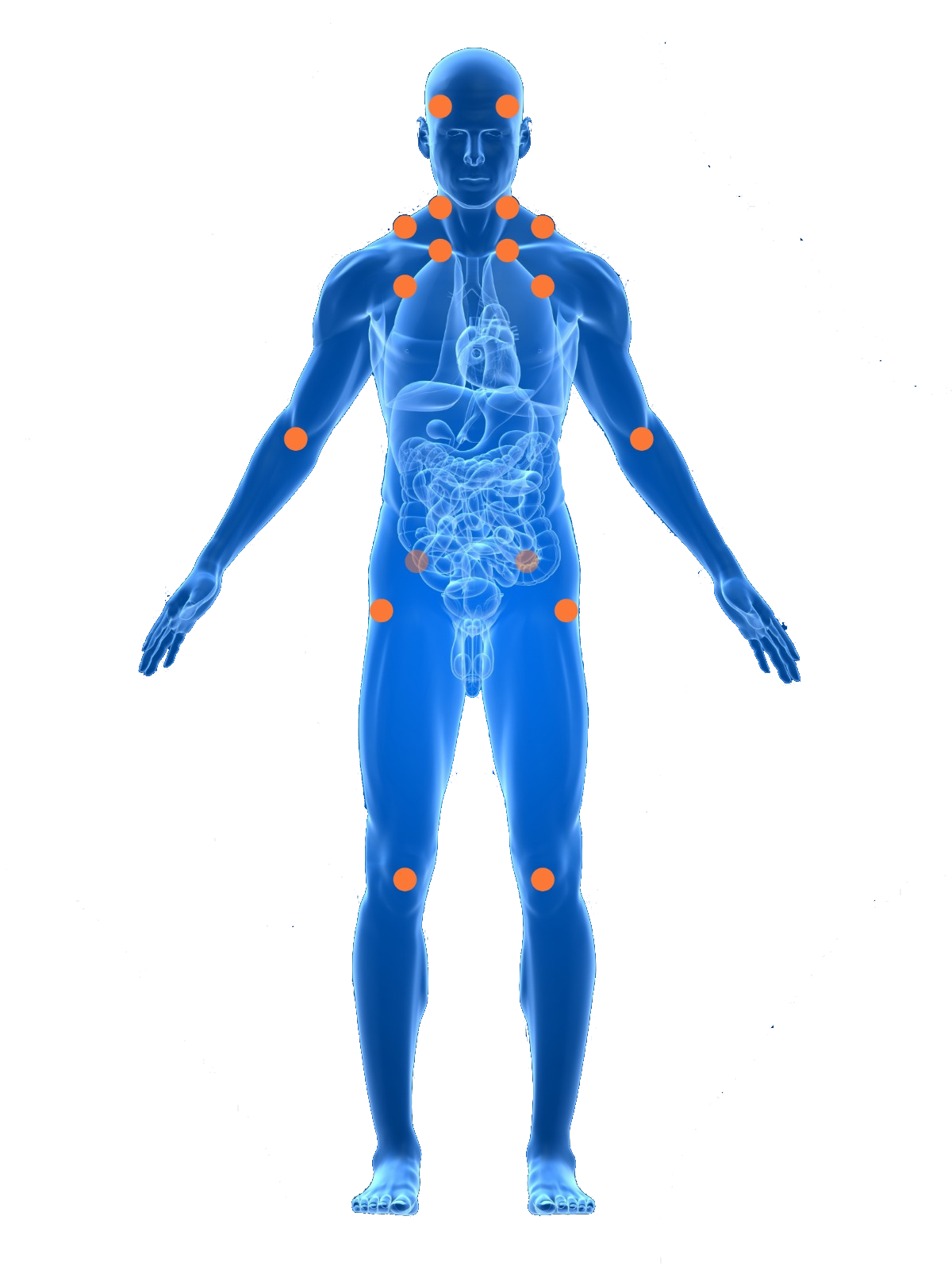
The 18 Tender Point Locations
Tender points in fibromyalgia are specific anatomical sites where applied pressure produces intense, disproportionate pain. They occur in bilateral pairs (left and right sides of the body), giving a total of 18 possible points across 9 regions. These are distinct from trigger points seen in myofascial pain syndrome.
| # | Region | Exact Location |
|---|---|---|
| 1–2 | Back of the Neck (Suboccipital) | On the left and right side of the back of the neck, directly below the hairline, where the neck muscles insert into the base of the skull |
| 3–4 | Front of the Neck (Low Cervical) | On the left and right side of the front of the neck, above the collarbone (clavicle), over the lower cervical vertebrae (C5–C7) |
| 5–6 | Upper Chest (Second Rib) | On the left and right side of the chest, right below the collarbone, at the junction of the second rib and sternum (costochondral junction) |
| 7–8 | Shoulder / Upper Trapezius | On the left and right side of the upper back, near where the neck and shoulder join, over the midpoint of the upper trapezius muscle |
| 9–10 | Upper Back (Supraspinatus) | On the left and right side of the spine in the upper back, between the shoulder blades (scapula), at the origin of the supraspinatus muscle above the medial scapular spine |
| 11–12 | Inner Elbow (Lateral Epicondyle) | On the inside of either arm, where it bends at the elbow, 2cm distal to the lateral epicondyle, in the muscle belly rather than the joint itself |
| 13–14 | Lower Back (Gluteal) | On the left and right side of the lower back, right below the waist, in the upper outer quadrant of the buttock, over the gluteal muscle |
| 15–16 | Hip / Greater Trochanter | On either side of the buttocks, right under the hip bones, posterior to the greater trochanteric prominence of the femur |
| 17–18 | Knees (Medial Fat Pad) | On either kneecap, over the medial fat pad, just proximal to the joint line on the inner aspect of the knee |
Medical History and Physical Examination
A thorough diagnosis at Singapore Paincare involves more than tender point testing. Your pain specialist will take a detailed personal and family medical history, including:
- Onset, duration, and pattern of pain — including aggravating and relieving factors
- Sleep quality and fatigue levels
- Psychological profile — including history of stress, trauma, anxiety, or depression
- Any recent weight changes, physical injuries, or infectious illnesses
- Current and previous medications, including supplements and over-the-counter remedies
- Family history of fibromyalgia or other chronic pain conditions
Physical examination includes pressing on all 18 tender point sites and inspecting nails, skin, mucous membranes, joints, spine, and muscles to rule out arthritis, thyroid disease, and other structural disorders.
Laboratory Tests and Conditions That Must Be Ruled Out
In most cases of fibromyalgia, blood tests return normal results — and this is actually a useful diagnostic indicator. Abnormal results point toward another primary condition. Blood tests typically ordered include:
- Full blood count (FBC)
- Thyroid and liver function tests
- Inflammatory markers — ESR and CRP
- Autoimmune antibody panels (rheumatoid factor, ANA, anti-dsDNA)
- Sedimentation rate and uric acid levels
Conditions that must be excluded before confirming a fibromyalgia diagnosis include rheumatoid arthritis, systemic lupus erythematosus (SLE), Hashimoto’s thyroiditis, polymyalgia rheumatica, chronic fatigue syndrome, multiple sclerosis, Lyme disease, and viral conditions such as hepatitis and HIV. Psychological evaluation may also be recommended where laboratory results are inconclusive.
What Are the Treatment Options for Fibromyalgia?
Because fibromyalgia has multiple contributing causes — neurological, physiological, sleep-related, and psychological — it responds best to a multi-dimensional treatment approach. At Singapore Paincare, this is structured through the Painostic® methodology, which identifies the specific drivers of each patient’s pain before designing a personalised treatment plan.
The Painostic® Approach to Fibromyalgia
Developed by Dr. Bernard Lee Mun Kam, Painostic® is Singapore Paincare’s proprietary diagnostic framework. It assesses pain across four dimensions — ensuring treatment targets root causes, not just surface symptoms.
Pain Patterns
How pain behaves — timing, triggers, radiation, and aggravating factors that reveal underlying mechanisms.
Pathology
Structural or physiological changes assessed through clinical examination, imaging, and diagnostic nerve blocks.
Pain Perception
Identifying central sensitisation and functional overlays — how the nervous system amplifies pain signals.
Psychology
Cognitive, emotional, and behavioural dimensions — fear-avoidance, catastrophising, and mood disorders that perpetuate the pain cycle.
Minimally Invasive Procedures to Fibromyalgia
Where appropriate, Singapore Paincare’s pain specialists use minimally invasive procedures to interrupt the pain cycle directly — without surgery, without hospital admission, and with minimal downtime. These procedures bridge the gap between conservative therapy and open surgery, targeting the root source of pain rather than masking it.
A targeted mixture of local anaesthetic, anti-inflammatory, and muscle relaxant delivered to the affected site to stop muscle spasm and reduce neurogenic inflammation at the source. Particularly effective for the neck, shoulder, and upper back muscle groups most affected by fibromyalgia.
A regenerative procedure using the patient’s own concentrated platelets to stimulate healing via a controlled, temporary low-grade inflammatory response — promoting tissue repair and growth in affected soft tissue regions.
Pharmacotherapy
Standard NSAIDs and opioids are generally not effective for fibromyalgia and are not the primary approach at Singapore Paincare. Instead, medications are selected for their ability to modulate the nervous system and interrupt the central sensitisation cycle:
| Medication Class | Role in Fibromyalgia |
|---|---|
| Anticonvulsants (Gabapentin, Pregabalin) | Nerve stabilisers that reduce abnormal pain signal transmission and help improve sleep quality |
| Low-dose Antidepressants (Amitriptyline) | Pain modulation, muscle relaxation, and sleep improvement, used at sub-antidepressant doses |
| Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs) | Address both pain perception and the mood disturbances commonly associated with fibromyalgia |
| Anti-inflammatories (Diclofenac, Celecoxib) | Used selectively where peripheral inflammatory components are contributing to symptoms |
Cognitive Behavioural Therapy (CBT)
Fibromyalgia is not “all in the mind” — but psychological factors significantly influence how pain is experienced and managed. CBT is an evidence-based component of fibromyalgia treatment that helps patients:
- Reframe pain-related thought patterns and reduce fear-avoidance behaviour
- Build pacing strategies to avoid the overexertion-collapse cycle common in fibromyalgia
- Improve sleep hygiene and stress regulation
- Reduce reliance on unhelpful medications and increase functional capacity
Interdisciplinary treatment programmes that include CBT have been shown to produce significant pain improvement in up to 42% of fibromyalgia patients, with effects persisting for at least six months.
Exercise and Rehabilitation
Supervised, graduated exercise is one of the most effective long-term strategies for fibromyalgia. Low-impact aerobic activity — including walking, swimming, and stationary cycling — raises the pain threshold and reduces fatigue over time. Patients are advised to start gradually and increase intensity progressively, as premature high-intensity exercise can temporarily worsen symptoms.
Who Is Most at Risk of Fibromyalgia?
Fibromyalgia affects an estimated 2–5% of the global population. Risk is not evenly distributed:
| Risk Factor | Detail |
|---|---|
| Sex | 80–96% of diagnosed patients are female; symptoms are typically more severe in women than men |
| Age | Most common between ages 35–55, though fibromyalgia can occur at any age including in children |
| Family history | First-degree relatives of fibromyalgia patients have significantly elevated risk |
| Existing rheumatic disease | Patients with rheumatoid arthritis or lupus are at higher risk of concurrent fibromyalgia |
| Trauma and infections | Physical injuries, viral infections (dengue, pneumonia), and emotional trauma can trigger onset |
Fibromyalgia Specialist at Singapore Paincare
Dr. Bernard Lee Mun Kam 李文鉴医生
Founder & Senior Consultant Pain Specialist | Singapore Paincare Center
MBBS (S’pore) | MMed (Anaesthesiology) | FFPMANZCA | Member, IASP | Member, PAS
Dr. Lee has over 20 years of clinical experience in pain management. He established the Chronic and Interventional Pain Management Service at Tan Tock Seng Hospital, founded Singapore’s first Women’s Pain Centre at KK Women’s and Children’s Hospital, and developed the Painostic® diagnostic methodology. He was quoted in The Straits Times & Silver Streak on fibromyalgia as a leading authority on the condition in Singapore.